2001-01-01 08:00:00
Epistemic status: fiction
This summer I was feeling that I lost my sense of purpose. So, I got really depressed. Then, I started to read a lot.
One of the books I read was an investigation into the appearance of consciousness in humans by Julian Jaynes, called The Origin of Consciousness in the Breakdown of the Bicameral Mind. The book was a curious one. In fact, it was so curious I decided I had to write a review of it. Part-review, part-critique, in the form of an essay slash blog post.
I write the first draft in under a week. I adore it. it exemplifies my wit, my writing talent, and my insightfulness in a cocktail which should probably be named “Sex on the Beach with Alexey”. So, I send it over to a friend.
He tells me that he got lost in the first paragraph and he’s not going to read any further. I think he must just be too dull to see its beauty. So, I send the essay to two more friends. The first one tells me that she’s read the first half and she feels that it’s “enough” for her. The other one tells me that she’s finished it and that it’s “ok”.
This is the point where I start to suspect that just maybe I will need to adjust a thing or two. This is also the point where you may start to wonder what the hell does this story have to do with tinder at all.
Coincidentally, I have a tinder date with a girl named L. coming up just a day after I finished the first draft and realized that I have three less friends. L. sports large glasses and flawless carré, and studies economics at my university. She’s also freakishly smart and absurdly hot. I’m just trying my best to look adequate next to her.
Somehow, our chat turns to books and this is where a revelation strikes me. The moment I see an opening, I start to recite the entire blog post I wrote yesterday to her. I can see that she’s trying her best to look interested. I can also see the strain on her face. But. By the variation in that strain I figure out exactly the parts of the post that need the most work.
After the date L. tells me that she’s sorry but she has no further romantic interest.
I chop up the post in pieces and rewrite it almost from the scratch.
Later that week I have agreed to meet up for drinks with another girl: M. She’s athletic and buzzing with energy. M. studies at a medical school and is planning to go on to get a PhD in molecular biology. While waiting for me in metro she was reading Thomas Mann’s The Magic Mountain. Of course, we move on to discuss The Glass Bead Game (which you should totally read if you haven’t yet, by the way). Another few moments later I see the opportunity and I strike: we spend the next half an hour talking about Jaynes. Most of the time her face vacillates between boredom and slight annoyance. But every now and then I see a spark of interest lighting up in her eyes.
After the date she tells me that she loved my sense of humor, but that I’m “not her type”.
I throw out about a third of the post and completely rewrite its intro.
Next week, another unsuspecting girl, V., steps right into my trap. Her jawline tells me about her assertiveness and her light blue eyes speak of the northern coast of France she recently returned from. We’ve been walking around and about the city center for the last 2 hours and eventually we end up discussing Gabriel García Márquez and Latin American magic realism. She found One Hundred Years of Solitude to be remarkable in its picturesqueness; I found it to be remarkable in its obsession with incest. But I’m getting sidetracked.
Slowly but surely, I start to retell her the latest iteration of my essay. She’s definitely immersed. Her eyes start to live up to their promise of la Manche’s excitability and I manage to make her engaged throughout the entire narrative. I realize that it has finally coalesced into something worthwhile.
A few days later she writes me that she wants to hang out some more.
I make a few minor edits and finally publish the post.
Thanks to Ann Taranina for reading early drafts of this post and offering helpful suggestions and to my twitter friend Anna for pointing out some typos.
A special thanks to all the girls from tinder who were forced to endure my ramblings on topics, including, but not limited to, Julian Jaynes, modern art, and general concerns about the aesthetics of the modern world.
This post was inspired by Steve Friedman’s Lost on Treasure Island and by Tal Yarkoni’s the weeble distribution: a love story.
2001-01-01 08:00:00
Links collections I’ve been reading:
Blake Byers on X:
GLP1s have added $1T in market cap to Eli and Novo over the last 5 years. That’s 3x+ the market cap created by all biopharma startups over the last 30 years combined. This is a bit of an indicment of the biotech startup ecosystem. There are many $1T and even $10T drugs to be invented, we just don’t fund them. Through no one persons fault, the biotech industry is stuck in a local performance maxima. Faced with lower multiples than tech, biotech funds have to pitch something other than straight multiple to LPs and the only other level is faster liquidity. Biotech has been good at this, with the average age of biotech companies at IPO being 2 years younger than tech companies at IPO (~5.5 years vs 7.5 years). This means biotech funds need to back companies that can get to IPO within a few years. This requirement constrains the types of companies funded by bio funds to ’linear bet’ plays (where you buy at some reasonable multiple based on current performance, etc). As any experienced venture fund manager will tell you, a portfolio of linear bets underperforms a portfolio of asymmetric bets. Double unfortunately, no one firm can break this model because no one firm is the sole backer of a company to profitability. You must rely on an ecosystem of capital partners. So if you are the one firm that strikes out and funds asymmetric companies, no one will show up to fund the company downstream and your whole portfolio will fail. For this reason, I think the biggest plays in bio over the coming decade will be mostly backed by generalist funds rather than bio funds. [emphasis mine]
*Note this will perpetuate the trend of sector specific funds underperforming generalist funds (by industry and geo!).
How to Stage a Coup - an interview of Edward Luttwak by Santi Ruiz:
Now for the megalomaniac explanation for what happened next, which was a very rapid decline in the number of coups. Coups had been very common until about two years after the book was published, and then stopped. The reason is that authorities everywhere reverse-engineered the book. The book was published in English, and it was immediately translated into about 13 languages. It went all over the place. I think what happened is that people learned to reverse engineer.
So, you have an armored mobile force, which is near the capital. I say, “Make sure either you move it 400 kilometers away, as far away as you can, or else make sure that it’s commanded by your son or nephew or something like that.” So they did that, they put their nephews in charge of any mobile force. My book caused a decline of coups.
Oxford Biologist Denis Noble: “The Fact Is that I Think Neo-Darwinism Is Dead”:
I respect Denis Noble and in disagreeing with him I do not mean to slight his deep insights into how biology works. I sincerely hope he continues in his work. But there’s an inherent tension between systems biology and any model that claims that life is ultimately the result of strictly blind and undirected material causes. That’s because in our normal experience, when we see purpose, function, and top-down design, this happens because it was emplaced by an intelligent mind who was there to give purpose to the system. In our experience, purpose does not arise by blind mechanism, or by accident. Denis Noble may disagree with me, but I suspect a lot of people — both friends and foes of intelligent design — won’t.
That realization was a dark moment of real despair, and I became terribly depressed. I felt hopeless, and isolated from my own family. I felt as if I had a shameful secret that I had to keep from them. Perhaps even worse, I felt isolated from a part of myself that I had loved dearly and that had made me happy. I felt like a person whom I could no longer like or respect.
Eventually, though, after at least a year in this kind of state, a truly wonderful thing happened. I remember very clearly: I was in the middle of a long, solo road trip, driving through the staggering mountains of Colorado along I-70 west of Denver. The radio didn’t work in my car, so I had nothing to do for entertainment but to provoke myself to internal argument. Suddenly, during the course of one of these arguments, and among the mountains of Colorado beneath a beautiful bright sky, I had an epiphany.
…
What I realized in that moment is that my happiness in life did not come from, or rely upon, any religious idea. It was not dependent on any particular idea of God or any specific narrative about my place in the universe. My feelings of being fundamentally safe and loved in the world were gifts that had been given to me by my family; even if I interpreted them in a religious way, they were never inherently religious feelings. Today I am just as capable as ever of feeling like a good and a happy person, even though I lack any absolute standard for “good” or any plausible ultimate source from whom that happiness flows. My religion had always taught me to credit its god for those feelings, but I realize now that they exist whether I believe in Him or not.
Never giving up is what makes us human.
The 47 Seconds That Saved Kamala Harris’s Political Career:
Nearly 14 years ago, Kamala Harris’s opponent in the California attorney general’s race gave an answer at a little-watched debate that was frank — and fateful for the future Democratic presidential nominee. …
“Everyone writes history like it’s all inevitable,” said Ms. Harris’s chief strategist in the 2010 race, Averell “Ace” Smith. Her first statewide win, he said, was anything but.
“That was as close to a near-death experience for a political career as you can get,” said Chris Jankowski, a Republican strategist who then led a national G.O.P. group that spent $1 million in a failed bid to end Ms. Harris’s career before it could really get started. “If she had lost that race, she would not be the nominee for president — no chance.”
How Vacations Affect Your Happiness:
The study, published in the journal Applied Research in Quality of Life, showed that the largest boost in happiness comes from the simple act of planning a vacation. In the study, the effect of vacation anticipation boosted happiness for eight weeks.
After the vacation, happiness quickly dropped back to baseline levels for most people.
The Alchemist and His Quicksilver by Alvaro De Menard:
We are going around the table on new year’s eve, rating our past year on a scale of 1 to 10. The guests: artists, fashion designers, jewelers, and one or two people with real jobs sprinkled in for diversity. Two immaculately groomed poodles run around and entertain the visitors. Before us, an exactingly curated procession of morsels: blini with salmon and caviar, black brioche with cured egg yolk and parmigiano foam, ravioli with pumpkin and cod with browned butter and crispy sage. The apartment, naturally, is luxurious without being gauche (that would be unforgivable) every piece selected with impeccable taste and just the right amount of personal touch. And so we rate our years, the numbers start coming out, and it is a parade of 2s and 3s, each delivered with a sort of practiced weltschmerz. One of the guests plans to commit suicide soon. The only 10 in the room: me. Is it because I’ve been perfectly happy, carefree? No—not quite.
I’ve been thinking a lot about this lately, about my relationship with suffering. All this pain in the past few months, I think most people would recoil from it. Instead, I’m drawn towards it. Is it psychological masochism? The intensity of emotion—it makes me feel alive, present, it gives me a heightened awareness of everything, inside and out.
I Built a Medieval Watermill to Power My Tools (YouTube)
The Challenge of Building New Cities: Inside The Satmar Hassidic Takeover of Bloomingburg by Dan Frank:
This is the story of how a community of Hassidic Jews, through subterfuge and electoral fraud, took over a small town in an attempt to make it their own
Michel Houellebecq: “Writing is like cultivating parasites in your brain.”
Michel Houellebecq: ‘People who have humanitarian ideas are a catastrophe’:
What is it, I ask, that has driven the rise of the French far right in the past 20 years? “Immigration,” he answers without hesitation. “And also, the total scorn of the elites.”
He’s speaking in a low voice, in short sentences interspersed with long pauses, every now and then popping mysterious pills from a plastic bag. He mentions the 2005 referendum on the European constitution. The result was “No”, later overridden by the French parliament. “It was almost 20 years ago and people still remember it,” he says. “They really made fools of us.”
“It’s dangerous to mock people,” he adds, and pauses. “I mean, you can mock them, but there are limits.”
never waste a motivated moment: “the 3am motivation dies the next morning when you wake up.”
Why can’t biology move faster? by Heidi Huang:
I suspect academia’s work culture is more moderate compared to SpaceX’s because, as mentioned above, biological processes set their own pace. When key processes simply cannot be accelerated, working around the clock offers diminishing returns. The cell culture that needs a week to grow won’t mature faster if you sleep under your desk.
The unpredictable, non-compressible timelines of biological processes create a bursty pattern of intense 50-60 hour weeks, followed by periods of 30-hour work weeks spent waiting for cells to grow and catching up on reading papers.
How Elon Musk Executed His Takeover of the Federal Bureaucracy:
Mr. Musk’s transformation of DOGE from a casual notion into a powerful weapon is something possible only in the Trump era. It involves wild experimentation and an embrace of severe cost-cutting that Mr. Musk previously used to upend Twitter — as well as an appetite for political risk and impulsive decision-making that he shares with President Trump and makes others in the administration deeply uncomfortable. …
Mr. Musk and his advisers — including Steve Davis, a cost cutter who worked with him at X and other companies — did not want to create a commission, as past budget hawks had done. They wanted direct, insider access to government systems. They realized they could use the digital office, whose staff had been focused on helping agencies fix technology problems, to quickly penetrate the federal government — and then decipher how to break it apart.
2001-01-01 08:00:00
Discuss this study on my forum or see discussion on Hacker News (>400 points, >350 comments).
Abstract
I slept 4 hours a night for 14 days and didn’t find any effects on cognition (assessed via Psychomotor Vigilance Task, a custom first-person shooter scenario, and SAT). I’m a 22-year-old male and normally I sleep 7-8 hours.
I was fully alert (very roughly) 85% of the time I was awake, moderately sleepy 10% of the time I was awake, and was outright falling asleep 5% of the time. I was able to go from “falling asleep” to “fully alert” at all times by playing video games for 15-20 minutes. I ended up playing video games for approximately 30-90 minutes a day and was able to be fully productive for more than 16 hours a day for the duration of the experiment.
I did not measure my sleepiness. However, for the entire duration of the experiment I had to resist regular urges to sleep and on several occasions when I did not want to play video games was very close to failing the experiment, having at one point fallen asleep in my chair and being awakened a few minutes later by my wife. This sleep schedule was extremely difficult to maintain.
Lack of effect on cognitive ability is surprising and may reflect true lack of cognitive impairment, my desire to demonstrate lack of cognitive impairment due to chronic sleep deprivation and lack of blinding biasing the measurements, lack of statistical power, and/or other factors.
I believe that this experiment provides strong evidence that I experienced no major cognitive impairment as a result of sleeping 4 hours per day for 12-14 days and that it provides weak suggestive evidence that there was no cognitive impairment at all.
I plan to follow this experiment up with an acute sleep deprivation experiment (75 hours without sleep) and longer partial sleep deprivation experiments (4 hours of sleep per day for (potentially) 30 and more days).
I’m wary of generalizing my results to other people and welcome independent replications of this experiment.
All scripts I used to perform statistics and to draw graphs, all raw data, and all configuration files for Aimgod (costs $5.99) and for Inquisit 6 Lab (has a 30-day trial) necessary to replicate the experiment are available on GitHub. Pre-analysis plan is available here and on GitHub.



The cumulative cost of additional wakefulness: dose-response effects on neurobehavioral functions and sleep physiology from chronic sleep restriction and total sleep deprivation Van Dongen H, Maislin G, Mullington JM, Dinges DF. The cumulative cost of additional wakefulness: dose-response effects on neurobehavioral functions and sleep physiology from chronic sleep restriction and total sleep deprivation. Sleep. 2003 Mar 1;26(2):117-26. is a study published in journal Sleep in 2003 by Hans P.A. Van Dongen, Greg Maislin, Janet M. Mullington, and David F. Dinges.
Since then it has become one of the most well-known experiments in sleep science, accumulating more than 2700 citations and having its findings enter the popular culture. In particular, it appears that the idea that people do not notice the cognitive impairment due to sleep deprivation and that sleeping 6 hours a night for two weeks is enough to produce significant cognitive impairment both originate from this study.
Intrigued by the study’s findings and having my interest in sleep science heightened by my investigation into Matthew Walker’s Why We Sleep, I decided to attempt to partially replicate and extend it.
There’s not much more to say about the prior literature on the subject as most of it is extremely low quality. In particular, I have been able to find exactly one pre-registered experiment of the impact of prolonged sleep deprivation on cognition. It was published in 2020 by economists from Harvard and MIT and found null effects, if data is analyzed according to the authors’ pre-analysis plan.
I gave myself a sleep opportunity of 8 hours (23:30-07:30) for 7 days prior to the experiment to make sure I don’t have any sleep debt carried over. My average sleep duration in these days (2020-03-27 to 2020-04-02) was 7.78 hours (standard error: 0.15 hours).
I slept for 4 hours a night (3:30-7:30) for 14 days (one of the experimental conditions in Van Dongen et al. 2003), with all other sleep being prohibited, and compared my cognitive abilities on days 12, 13, and 14 of sleep deprivation (treatment) to my normal state (control). I did not test myself every day because the cognitive deficits in the 4-hour condition were increasing monotonically in Van Dongen et al., and I was only interested in the most severe consequences of sleep deprivation.
I remained inside for the duration of the experiment. I worked, played video games, watched movies, browsed the internet, read, walked around the apartment, but did not engage in any vigorous activities. I avoided direct sunlight and turned off all lights during sleep times.
I did not use any caffeine, alcohol, tobacco, and/or medications in the 2 weeks before the experiment or during the experiment.
I only ate from 12pm to 8pm for the 2 weeks before the experiment and continued this schedule during the experiment. My diet was not otherwise restricted.
I do not have any medical, psychiatric or sleep-related disorders, aside from occasionally experiencing stress-related strain in my chest, and I did not experience any unusual symptoms during the experiment.
I worked neither regular night nor rotating shift work within the past 2 years. I have not travelled across time zones in the 3 months before the experiment.
I performed 3 tests: Psychomotor Vigilance Task, a custom Aimgod scenario (guzey_arena_0), and SAT.

Figure 4. Clips of tasks I performed in the experiment. Left: PVT. Center: guzey_arena_0. Right: SAT. Created with ezgif.com.
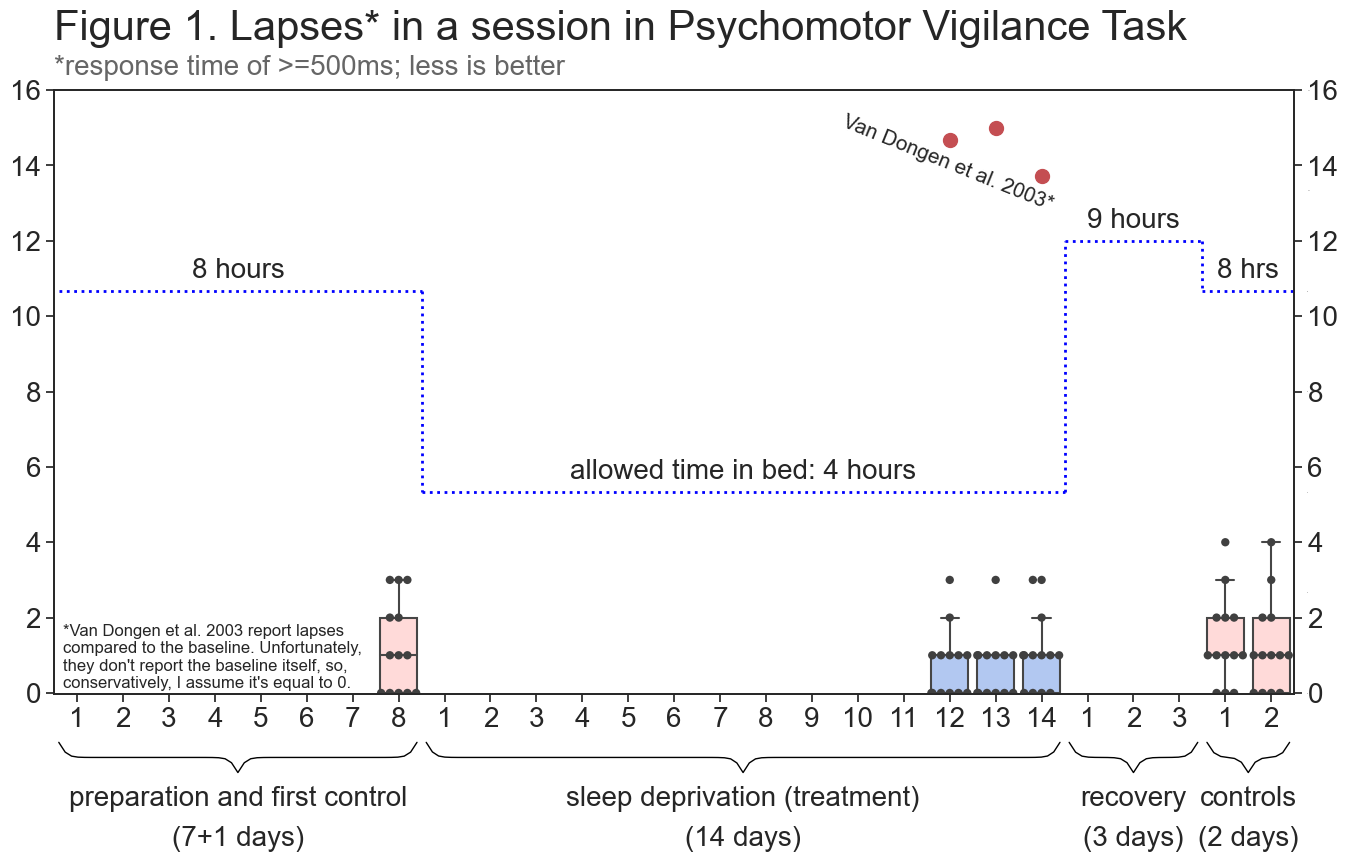
Psychomotor Vigilance Task is essentially a 10-minute-long reaction test that has become a standard way to assess wakefulness in sleep research. The standard way to analyze PVT data is to count the number of lapses (trials in which response time was >=500ms) in a session. This is how I analyzed the data.
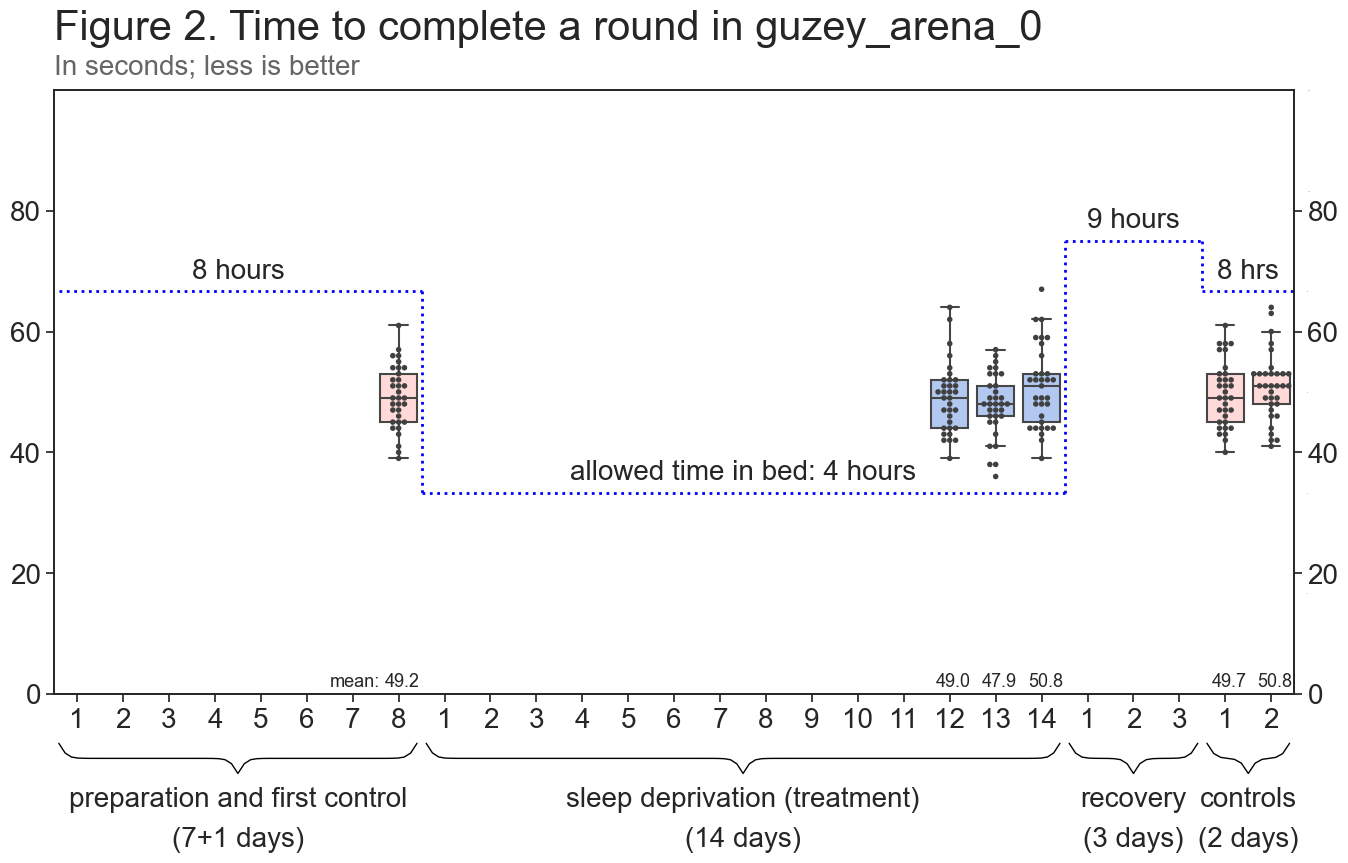
guzey_arena_0 is a first-person shooter scenario in which the player has to kill 20 bots running around the arena as quickly as possible (10 bots are present at a time and they respawn in a random location on kill). The scenario requires a mix of quick reaction time (bots frequently change directions and appear in random locations), tactical thinking (you have to choose which bot to pursue and where to look for them), and fine-motor skills (you have to move your around using the keyboard and aim accurately using the mouse).
guzey_arena_0 is the test I care the most about. I believe it’s superior to PVT for several reasons:
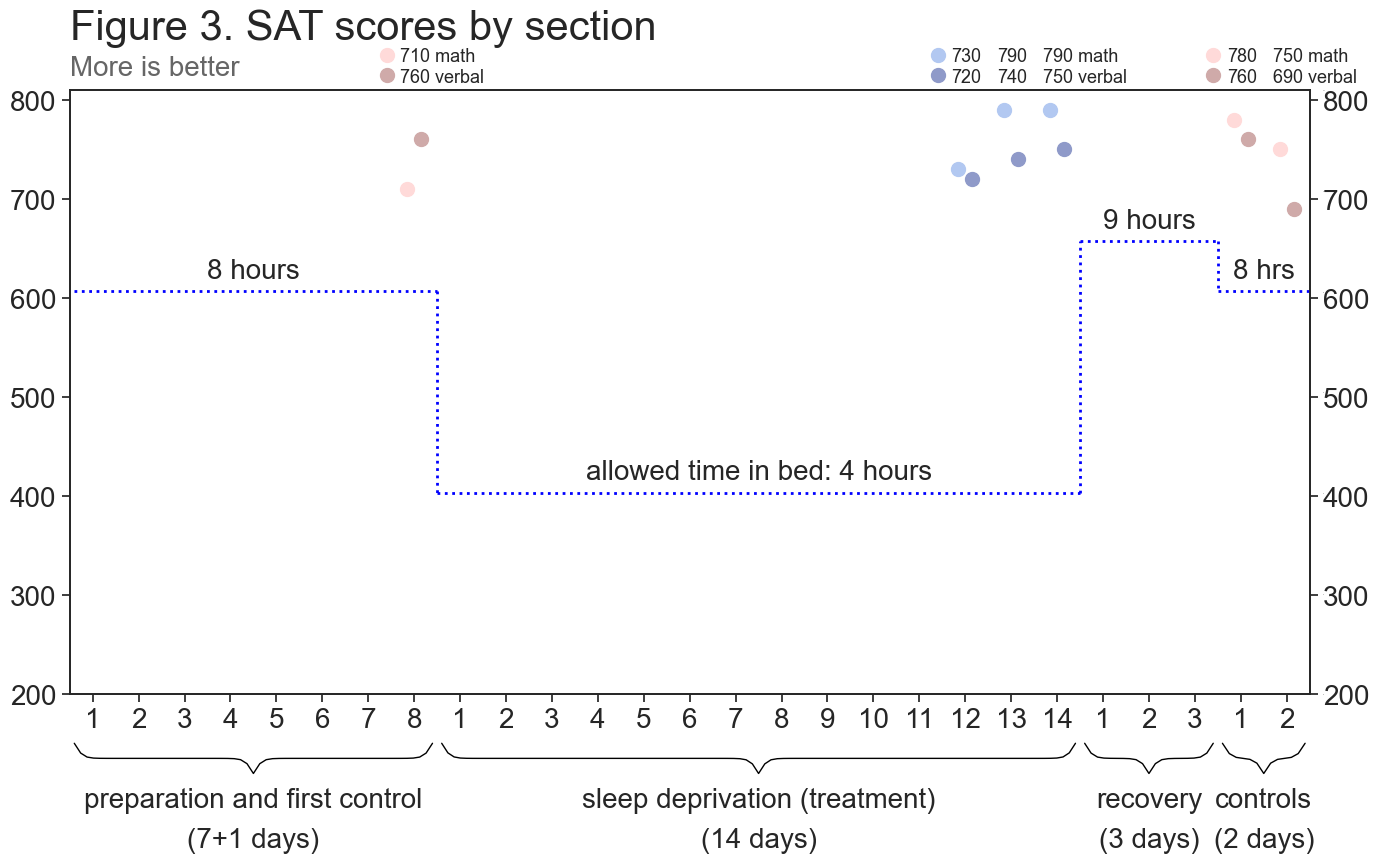
The SAT is a 3-hour-long composite test that consists of verbal (text comprehension, grammar, etc.) and math problems. It is the standard way to assess college preparedness in the US and is taken by million of high school students every year.
I took control measurements 1 day before starting sleep deprivation and on days 4 and 5 after I ended sleep deprivation. I took treatment measurements on days 12, 13, and 14 of sleep deprivation.
Data collection, as well as my strategy to deal with practice effects is described in detail in pre-analysis plan (PAP). All deviations from PAP are described in Discussion.
I performed paired t-tests for PVT and for guzey_arena comparing the means of treatment and control conditions at 0.025 significance level (0.05 significance level, Bonferroni-corrected for 2 comparisons) against a two-sided alternative.
In PAP, I wrote:
I will perform two two-tailed t-tests to compare means for both hypotheses at alpha=0.025.
I did not mention that t-tests will be paired t-tests, because I did not realize that t-tests for independent samples and for paired samples are different.
In PAP, I calculated the required sample sizes for PVT and for guzey_arena_0 to be able to detect an effect-size of 0.8 and 0.5 respectively, at 0.025 significance level and 0.895 power (0.895 power ensures that I achieve 0.8 joint power (probability to correctly reject both null hypotheses if they’re both false)).
The calculated sample size was 39 pairs of observations for PVT and 99 pairs of observations for guzey_arena_0. These are the sample sizes I collected.
However, these sample size calculations were incorrect. Because the power of a paired t-test is higher than of an independent samples t-test, it turned out that the effect-sizes I was able to detect for these sample sizes was 0.58 for PVT and 0.35 for guzey_arena_0 (at 0.025 significance level and 0.895 power).
Figure 5. Left: Cohen's d of 0.58. Right: Cohen's d of 0.35. Created with R Psychologist.
I am not performing any statistics on the SAT data, in light of extremely small number of observations.
I feel slightly weird that I’m only correcting for 2 comparisons, given that I’m discussing the SAT results, even though I’m not performing any statistics on them.
Control mean: 1.34; treatment mean: 1.12 (less is better).
Control median: 1.0; treatment median: 1.0 (less is better).
Control standard error: 0.12; treatment standard error: 0.11.
p-value: 0.18; t-value: 1.35. Not significant.
Summary: There was no statistically significant difference in my PVT performance between control and treatment conditions.

Control mean: 49.91; treatment mean: 49.24 (less is better).
Control median: 50.0; treatment median: 49.0 (less is better).
Control standard error: 0.54; Treatment standard error: 0.6.
p-value = 0.382; t-value = 0.879. Not significant.
Summary: There was no statistically significant difference in my guzey_arena_0 performance between control and treatment conditions.

Control scores (math,verbal): (710,760), (780,760) (750,690); treatment scores (math,verbal): (730,720), (790,740), (790,750) (more is better).

In PAP, I wrote:
My key hypothesis is that the number of lapses on PVT increases because it’s a boring as hell task. It’s 10 minutes just staring into the computer waiting for the red dot to appear periodically. So I think that sleep deprived are just falling asleep during the task but are otherwise functioning normally and their cognitive function is not compromised. Therefore, I expect that my PVT performance will deteriorate but Aimgod performance will not, since this is an interesting task, even though it primarily relies on attention for performance.
My first hypothesis was not confirmed. There was no difference in my PVT performance between control and treatment conditions. I thought that during the test I would start falling asleep and fall into microsleeps but it seems that video games – which I played whenever I was feeling too sleepy – stimulated me to the point that even doing a boring 10-minute-long test was not enough to induce microsleeps.
I believe that the quality of my PVT data is not very high. First, while I planned to take PVT at 7:40, 13:00, 13:20, 13:40, 16:00, 16:20, 16:40, 19:00 19:20, 19:40, 22:00, 22:20, 22:40, sometimes I forgot about it and sometimes I was busy during the designated time. As a result, even though I took the vast majority of tests within 5-10 minutes of designated time (largest delay: 22 minutes), I did not take PVT exactly on time. It could be argued that I strategically delayed my PVT sessions in order to take the test when I start feeling more alert. Further, I was extremely bored in the last 2 days of taking control measurements and sometimes got distracted and lost in thought, which resulted in me getting 3 and 4 lapses per session (as can be seen on Figure 1). I do not believe that these lapses represent my lack of alertness. Finally, I had to change the timing of last 3 tests on the last treatment day from 22:00, 22:20, 22:40 to 21:00, 21:20, 21:40 because I was going to bed at 22:00 and I did not account for this when writing the protocol (all such changes can be found here).
To conclude, I believe that PVT data strongly suggests that I was able to control my level of sleepiness for the duration of the experiment but I don’t think much else can be concluded from it. This interpretation seems to me to be robust, but I welcome any further criticisms that might challenge it.
I’m not sure. I don’t think that I have any mutations that make me need less sleep, given that I sleep 7-8 hours normally. I believe that the most plausible explanation is that my cognitive performance was just not affected by chronic loss of sleep that much.
It seems that there’s very high variation in how people respond to sleep deprivation. For example, Van Dongen et al. 2004 Van Dongen H, Maislin G, Dinges DF. Dealing with inter-individual differences in the temporal dynamics of fatigue and performance: importance and techniques. Aviation, space, and environmental medicine. 2004 Mar 1;75(3):A147-54. (a different paper by the same first author) find that:
As measured by performance lapses on a psychomotor vigilance task (13), some subjects were found to have much greater impairment from sleep loss than others (Fig. 1, left-hand panel). Thus, some subjects seemed to be relatively vulnerable to performance impairment due to sleep loss, while others seemed to be relatively resilient. Interestingly, vulnerable and resilient individuals did not differ significantly in the amount of sleep they felt they needed or routinely obtained, as assured by surveys and daily diaries. This suggests that inter-individual differences in vulnerability to sleep loss are not just determined by differences in sleep need (42).
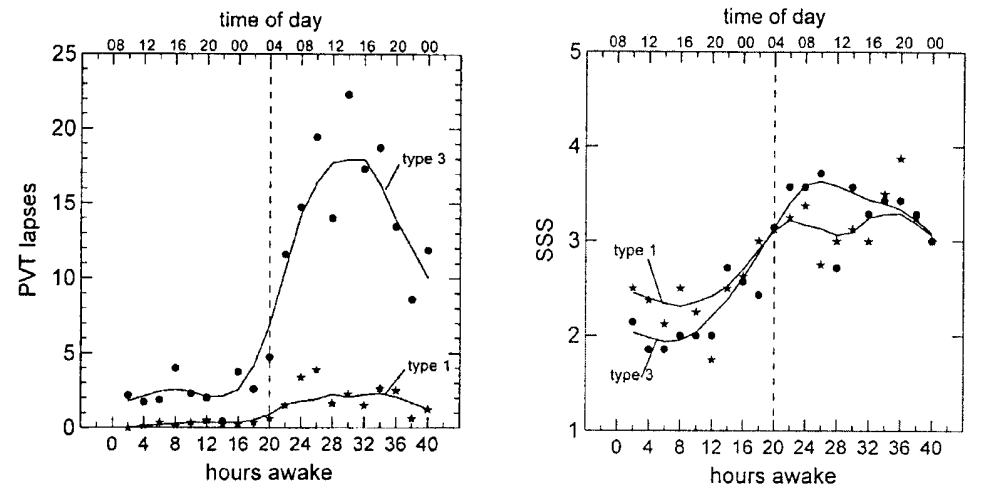
Figure 6. Neurobehavioral performance lapses on a psychomotor vigilance task (PVT; left-hand panel) and subjective sleepiness score on the Stanford Sleepiness Scale (SSS; right-hand panel) during 40 h of total sleep deprivation in a laboratory environment (11). Stars show PVT performance lapses and SSS sleepiness scores for the eight subjects most resilient to sleep loss (type 1); dots show the data for the 7 subjects most vulnerable to sleep loss (type 3). Despite the considerable difference in psychomotor performance impairment, there was no statistically significant difference in the profile of sleepiness scores between these two groups. Reprinted from Van Dongen et al. 2004.
My second hypothesis was confirmed. There was no difference in my guzey_arena_0 performance between control and treatment conditions.
I believe that the quality of my guzey_arena_0 data is high. I took tests in the same environment and was virtually always fully focused on them. Like with PVT, I performed the tests only approximately at the planned time (almost always within 5-10 minutes of the scheduled time). Also like with PVT, I had to change the time I took some of the tests at because I forgot to account for me going to bed earlier in the last 6 days of the experiment (all such changes can be found here). During one of the treatment sessions I accidentally took 12 samples. I discovered that I miscounted the number of samples I took in that session when I was extracting the data from the video and did not include sample 12 in the data, since the paired sample t-test I use relies on data being matched and my plan was to collect precisely 11 samples in each session. Even when including that sample, the control mean remains non-significantly higher than treatment mean.
To conclude, I believe that guzey_arena_0 strongly suggests that there was no major cognitive deterioration in the treatment condition. I believe that it provides moderate evidence that there was no moderate cognitive deterioration in the treatment condition. I believe that it is weakly suggestive evidence that there was no cognitive deterioration at all in the treatment condition.
In contrast to guzey_arena_0, the SAT has an absolute ceiling (800 on each section), which I know I’m able to approach (at least for the math section), thus creating an implicit control condition and making it immune to the effect of me consciously or unconsciously trying to suppress my control performance. This means that hitting a score in the vicinity of 800 on the math section and somewhere between 700 and 750 on the verbal section is a pretty good evidence of lack of major cognitive deterioration.
I ended up getting (730,720), (790,740), and (790,750) on (math,verbal) sections of SAT on days 12, 13, and 14 of treatment and getting (710,760), (780,760), and (750,690) on control days. The first low control score on the math section is a result of lack of practice and me running out of time after getting stuck on a question. The last low control score on the verbal section is a result of me becoming very bored with taking the SAT 5 days in a row, getting lost in thought for 10 minutes, and having to rush.
To conclude, I believe that the SAT data strongly suggests that there was no major or moderate cognitive deterioration in many aspects of my cognition, given that test includes challenging (to me) reading comprehension questions and requires quick mathematical thinking. I believe that it provides barely any evidence regarding minor cognitive deterioration, given that I usually end up having free time at the end of every section, which I use to double check my responses, and minor cognitive deterioration could result in me getting roughly the same score but with less time left.
I was fully alert (very roughly) 85% of the time I was awake, moderately sleepy 10% of the time I was awake, and was outright falling asleep 5% of the time. Subjectively, I felt that I gained somewhere between 2 and 3 hours of productive time every day.
Further, it appears that my sleep debt was not increasing over time. My impression is that during acute sleep deprivation, as one doesn’t sleep for 70+ hours, most stimulation ceases to work, meaning that video games are no longer able to bring one back to full alertness. In contrast to that, I found that I was able to go from “falling asleep” to “fully alert” at all times by playing video games for 15-20 minutes. I ended up playing video games for approximately 30-90 minutes a day.
Finally, even though I felt no cognitive deterioration and no accumulating sleep debt, maintaining this sleep schedule was incredibly hard. I had to resist regular urges to sleep and on several occasions when I did not want to play video games was very close to failing the experiment, having at one point fallen asleep in my chair and being awakened a few minutes later by my wife. Occasionally, when I tried to see if I could regain full alertness without video games, I would fall into a series of several-seconds-long microsleeps. I do not feel that I would’ve been able to maintain this schedule for these 14 days, had I not committed so hard to it by spending so much time designing it and publicly announcing my experiment.
In the evening of day 10 of treatment I had a call with a friend whom I talk to regularly. We spent an hour discussing strengths and weaknesses of several academic papers. For the majority of the conversation I was functioning at the peak of my ability, having to constantly engage with complex arguments and to do a lot of thinking on the fly, which taxed my long-term memory, short-term memory, logical thinking, and speaking ability. After the call I asked that friend if he noticed that I’d been sleeping for 4 hours a night for 10 days. He wrote:
lol
Did not notice
My roommate, who knew about my experiment, asked me how long I will continue to sleep for 4 hours a night after I had 2 nights of recovery sleep, meaning that he did not notice any significant changes in my state after I stopped being sleep deprived. I usually talk to him for 30-60 minutes a day.
I like being awake and I do not like sleeping. Thus, I was motivated to find the absence of effect of sleep deprivation on cognition. This might have resulted in me trying less hard in the control condition, compared to treatment condition. Unfortunately, I do not know how to blind myself to the amount of sleep I get. I discussed the lack of blinding in the context of this experiment in subsection SAT.
I care about even the smallest changes in my cognitive ability due to sleep deprivation. For example, if the effect-size is “only” 0.1, I still care about it. However, in order to detect such effect in this experiment, I would have had to spend more than 40 hours collecting 1224 pairs of observations for guzey_arena_0.
The situation would not look much better if I ditched PVT and only performed guzey_arena_0. In this case, I would need to collect 787 pairs of observations to detect effect-size of 0.1 at 0.05 alpha and 0.8 power.
Figure 6. Cohen's d of 0.1. Created with R Psychologist.
Although I did not experience any physical deterioration during the experiment, I did not track my health very rigorously.
It might be possible that sleeping 4 hours a night is unhealthy for the body or unhealthy for the mind over the long-term but the damage accumulates slowly and could not be noticed over a 14-day experiment.
I would like to thank Gleb Posobin, Drake Thomas, and Nabeel Qureshi for reading drafts of this study. I would like to especially thank Anastasia Kuptsova (for waking me up when I fell asleep during the day) and Misha Yagudin (for improving the plots immeasurably and many other helpful suggestions),
I would like to thank Tyler Cowen’s Emergent Ventures, Kyle Schiller and Adam Canady for the financial support of my writing and research.
I would like to thank Millisecond Software for providing me with a discount for Inquisit Lab 6, which I used to perform PVT.
In academic work, please cite this study as:
Guzey, Alexey. The Effects on Cognition of Sleeping 4 Hours per Night for 12-14 Days: a Pre-Registered Self-Experiment. Guzey.com. 2020. Available from https://guzey.com/science/sleep/14-day-sleep-deprivation-self-experiment/.
Or download a BibTeX file here.
Q:
In your November 2019 tweet announcing your Why We Sleep post you wrote:
For the last two months I’ve been sleeping for 4 hours a night
Why was this not mentioned in the post? Seems that it would provide important context for the experiment, given that your organism might have developed some sort of an adaptation to sleep deprivation.
A:
This tweet was a joke. I never slept 4 hours a night for more than a couple of days prior to the experiment. I experimented with sleep in 2019-2020 but it was not rigorous and I was never able to sleep less than 6-7 hours a day consistently. As mentioned above, when I don’t restrict sleep, I sleep 7-8 hours a night.
Also available (with the ability to view all changes since first publication) on GitHub.
This is the protocol for my sleep experiment that I will start on 2020-04-03. I will sleep 4 hours per night for 2 weeks and evaluate the effects of doing so on my cognition using psychomotor vigilance task (essentially, a reaction test), SAT (a 3 hour test that involves reading and math), and Aimgod custom scenario I called guzey_arena_0 (video) (this is a first-person shooter trainer game that allows the creation of custom scenarios. The scenario I created requires constant attention, eye-hand coordination, tactical thinking).
(inspired by Van Dongen et al 2003 https://academic.oup.com/sleep/article/26/2/117/2709164)
I’m going to remain inside throughout the experiment and my behavior will be monitored by my wife between 07:30-23:30 every day and will not be monitored between 23:30-03:30. I will check in in a google sheet every 15 minutes during that time to confirm that I’m not sleeping. I will work, play video games, watch movies, browse the internet, read, walk around the apartment, but will not engage in any vigorous activities. I will avoid direct sunlight and will turn off all lights during sleep times. I did not use any caffeine, alcohol, tobacco, and/or medications in the 2 weeks before the experiment. I do not have any medical, psychiatric or sleep-related disorders, aside from occasionally experiencing stress-related strain in my chest, and I will write down any unusual symptoms I experience during the experiment. I worked neither regular night nor rotating shift work within the past 2 years. I have not travelled across time zones in the 3 months before the experiment.
Days -7 to -1 (2020-03-27 to 2020-04-02): adaptation.
I will give myself a sleep opportunity of 8 hours (23:30-07:30) for 7 days prior to the experiment to make sure I don’t have any sleep debt carried over. My average sleep duration in these days (2020-03-27 to 2020-04-02) was INPUT with the standard deviation of INPUT.
Day -1 (2020-04-02): practice
I will give myself a sleep opportunity of 8 hours (23:30-07:30). I will practice the tasks I’m going to use in order to mitigate the most extreme practice effects during the experiment. I will perform all tasks as follows:
Days 1 (2020-04-03), 19 (2020-04-21), 20 (2020-04-22): control.
I will give myself a sleep opportunity of 8 hours (23:30-07:30). I will perform all tasks on these days as follows:
Days 2 to 12 (2020-04-04 to 2020-04-14): sleep deprivation
I will give myself a sleep opportunity of 4 hours (03:30-07:30). I will not test myself on days 2 to 12.
Days 13-15 (2020-04-15 to 2020-04-17): sleep deprivation, testing
I will perform all tasks on days 13, 14, 15 as follows:
Days 16-18 (2020-04-18 to 2020-04-20): recovery
I will give myself a sleep opportunity of 9 hours (22:30-07:30). I will not test myself on days 16-18.
I will test two statistical hypotheses in the study:
Effect sizes sleep-deprived number of lapses on PVT have previously been reported to be huge. In particular, Basner and Dinges 2011 report:
Effect sizes were high for both TSD (1.59–1.94) and PSD (0.88–1.21) for PVT metrics related to lapses and to measures of psychomotor speed
with PSD meaning that participants were allowed to sleep for 4 hours a night for 5 days. Studies show that the effect increases monotonically with an increase in the length of sleep deprivation (e.g. Van Dongen et al 2003), so we expect that the effect of sleeping for 4 hours a night for 2 weeks will be larger than this.
To be on the safe side, I’m going to collect enough PVT samples (n=39 control; n=39 experimental) to detect an effect size of 0.8 with 97.5% confidence level and 89.5% power.
I will collect enough Aimbot samples (n=99 control; n=99 experimental) to detect an effect size of 0.5 (medium-size effect) with 97.5% confidence level and 89.5% power.
Note that 97.5% confidence level is standard 95% confidence level Bonferroni corrected for 2 comparisons and that 89.5% ensures that we achieve 80% joint power (probability to correctly reject both null hypotheses if they’re both false).
I expect that practice effects will accumulate monotonically with performance of SAT and Aimgod, therefore I’m trying to equalize the average practice effects between control and experimental conditions. (control: day 1 (low practice), 19 (medium practice), 20 (high practice); experimental: day 13 (medium practice), day 14 (medium practice), day 15 (medium practice))
PVT is resistant to practice effects.
Statistical tests
I will perform two two-tailed t-tests to compare means for both hypotheses at alpha=0.025.
I’m taking the SAT as a curiosity, will collect very few samples and will not perform any statistical analysis on them.
Pre-registering my hypotheses
As Krause et al 2017 write in their review for Nature Reviews Neuroscience:
One cognitive ability that is especially susceptible to sleep loss is attention, which serves ongoing goal-directed behaviour4. Performance on attentional tasks deteriorates in a dose-dependent manner with the amount of accrued time awake, owing to increasing sleep pressure5,6,7. The prototypic impairments on such tasks are known as ’lapses’ or ‘microsleeps’, which involve response failures that reflect errors of omission4,5,6. More specifically, attentional maintenance becomes highly variable and erratic (with attention being sustained, lost, re-established, then lost again), resulting in unstable task performance4
My key hypothesis is that the number of lapses on PVT increases because it’s a boring as hell task. It’s 10 minutes just staring into the computer waiting for the red dot to appear periodically. So I think that sleep deprived are just falling asleep during the task but are otherwise functioning normally and their cognitive function is not compromised. Therefore, I expect that my PVT performance will deteriorate but Aimgod performance will not, since this is an interesting task, even though it primarily relies on attention for performance.
I will record the data and will not look at it until after the data collection is over to try to minimize the effect of my expectations on my performance. I will partially be able to see my performance level at Aimgod while performing it but will try not to do it…
Why are you not testing memory, executive function, mental rotation, creative reasoning…?
The more hypotheses I have, the more samples I need to collect for each hypothesis, in order to maintain the same false positive probability (https://en.wikipedia.org/wiki/Multiple_comparisons_problem). This is a n=1 study and I’m barely collecting enough samples to measure medium-to-large effects and will spend 10 hours performing PVT. I’m not in a position to test many hypotheses at once.
2001-01-01 08:00:00
I ask a lot of people about their life plans. At least half of them tell me that they have no idea where to move and are just coasting along, not sure what to do next. Therefore, this post.
More ideas
Emailing people you don’t know can be shockingly effective.
There’s an unwritten rule that you shouldn’t do it, but if you actually provide value you can connect with almost anyone instantly and for free.
Cold emails and twitter are a godsend for people who have high potential, but lack the opportunity to realize it. A few emails or tweets to a person you don’t know can literally change your life (they changed mine for sure!)
If you can demonstrate that you have high potential and/or can be useful to somebody, you should just email/tweet them and let them know about it. If you’re thinking “well, I’m not impressive enough” you’re likely wrong.
Here are two examples of my cold emails that worked: first, second. It appears that 20-50% of cold emails end up getting answered and while the experience can be nerve-wrecking and confidence-destroying, ultimately, it pays off.
(if you think that I’m good at writing cold emails - it wasn’t always like that. e.g. here’s one I wrote when I was 19 to a professor in my university I didn’t know and here’s one that I wrote to someone on the internet when I was 15; I’m super embarrassed by them and I’m fortunate that I got replies)
Also see my How to make friends over the internet, Follow Up, Why You Should Join Twitter Right Now.
Many projects only require you to have a computer and some free time. Some actually require funding. For them, see:
Nadia Eghbal’s list of microgrants
Harshita Arora’s List of opportunities, grants, fellowship programs, contests and things like that for young ambitious people
Thiel Fellowship: $100,000 for people under 23 “who want to build new things instead of sitting in a classroom”
Einstein Fellowship is “a fellowship for outstanding young thinkers who wish to pursue a project in a different field from that of their previous research.”
Emergent Ventures “seeks to support entrepreneurs and brilliant minds with highly scalable, “zero to one” ideas for meaningfully improving society”
And if you’re starting a company, then you can try to get more conventional VC funding.
How to Do What You Love by Paul Graham:
Another test you can use is: always produce. For example, if you have a day job you don’t take seriously because you plan to be a novelist, are you producing? Are you writing pages of fiction, however bad? As long as you’re producing, you’ll know you’re not merely using the hazy vision of the grand novel you plan to write one day as an opiate. The view of it will be obstructed by the all too palpably flawed one you’re actually writing.
“Always produce” is also a heuristic for finding the work you love. If you subject yourself to that constraint, it will automatically push you away from things you think you’re supposed to work on, toward things you actually like. “Always produce” will discover your life’s work the way water, with the aid of gravity, finds the hole in your roof.
Dive in by Nate Soares:
In my experience, the way you end up doing good in the world has very little to do with how good your initial plan was. Most of your outcome will depend on luck, timing, and your ability to actually get out of your own way and start somewhere. The way to end up with a good plan is not to start with a good plan, it’s to start with some plan, and then slam that plan against reality until reality hands you a better plan.
There’s no speed limit. by Derek Sivers:
But the permanent effect was this: Kimo’s high expectations set a new pace for me. He taught me “the standard pace is for chumps” — that the system is designed so anyone can keep up. If you’re more driven than “just anyone” — you can do so much more than anyone expects. And this applies to all of life — not just school.
Advice for ages 10-20 by Patrick Collison:
- To the extent that you enjoy working hard, do. Subject to that constraint, it’s not clear that the returns to effort ever diminish substantially. If you’re lucky enough to enjoy it a lot, be grateful and take full advantage!
- Make friends over the internet with people who are great at things you’re interested in. The internet is one of the biggest advantages you have over prior generations. Leverage it.
Career advice by /u/Kinoite:
Being at the Top of B-Tier will sufficient to get you a job. But, you’re probably screwed already. And, even if you’d gotten into a better school, trying to “Win” the Best-of-B-Tier competition is a stupid waste of time and money.
Instead, you want: (1) A professional accomplishment (2) that’s not part of your classes and (3) is acknowledged by a professional in your field.
So, I’ve invented The Working Resume™. It doesn’t list your academic credentials or any of your prior employers. It doesn’t show any of your past experience and it doesn’t list any jobs you ever did. No accomplishments, no achievements or awards. (Blasphemous, isn’t it?) So, what do you put on it?
- A clear picture of the business of the employer you want to work for.
- Proof of your understanding of the problems and challenges the employer faces.
- A plan describing how you would do the work the employer needs done.
- An estimate of what/how much you think you could add to the bottom line.
Things Many People Find Too Obvious To Have Told You Already by Patrick McKenzie:
Companies find it incredibly hard to reliably staff positions with hard-working generalists who operate autonomously and have high risk tolerances. This is not the modal employee, including at places which are justifiably proud of the skill/diligence/etc of their employees. …
Weak-form efficients market hypothesis is a good heuristic for evaluating the public markets but a really, really bad heuristic for evaluating either technical or economic facts about tech companies, startups, your career, etc etc. Optimizations are possible; fruit hangs low.
A Career Cold Start Algorithm by Andrew Bosworth
Don’t End The Week With Nothing (a) by Patrick McKenzie
I’ll close with my usual advice to peers: reading this email was valuable (knock on wood). Watching Jason’s video is valuable. Rolling up your sleeves and actually shipping something is much, much more valuable. If you take no other advice from me ever, ship something. You’ll learn more shipping a failure than you’ll learn from reading about a thousand successes. And you stand an excellent chance of shipping a success – people greatly overestimate how difficult this is.
Just don’t end the week with nothing.
See your Career as a Product (a):
Other product tropes also apply to careers: Capitalize on unfair advantages, insights, or relationships. Disrupt orthogonally, often from below—try not to compete head on. When you’re younger, take more market risk; when you’re more experienced, take execution risk.
However, certain mistakes product builders make also carry over to careers — namely, focusing on acquisition instead of retention (focusing on networking instead of relationships & reputation). Or working in a space that doesn’t get more valuable over time (e.g working in a dying industry), or building another “me-too” product without differentiation (not taking enough career risk).
“I often look at people’s achievements and think: I wish I’d done that. More rarely, I see the work that went into those achievements and think: I wish I were doing that. Chase the latter.” (a)
All the evidence-based advice we found on how to be successful in any job by Benjamin Todd on 80,000 Hours
How to Maximize Serendipity by David Perell
HOWTO: Be more productive by Aaron Swartz
Jacob Trefethen’s Vigilante accountability project
2001-01-01 08:00:00
My friends often ask me: what impact has New Science had? What impact has Emergent Ventures, which I admire so much, had? What impact will [project I’m currently thinking about] have?
There’s a few universally-considered truly great men: Alexander the Great, Julius Caesar, Napoleon. Here’s my question: did they have a positive impact on the world or negative?
I spent a lot of time studying each one of them and I have no idea.
What hope do we have to know what impact our actions, infinitesimally as meaningful as their were, will have on the course of history? There’s none. And anyone who tells you otherwise is lying.
Imagine asking Martin Luther what impact translating the Bible into vernacular German would have. Or imagine trying to estimate the impact of it 50 years after the Reformation started. The main result at that point was all kinds of crazy religious sects popping up and non-stop religious wars. But in the long-term, does anyone wish there was no Reformation?
Let’s go crazier. No Black Death – no industrial revolution. No Marx – no Ayn Rand. No Hitler – no Israel. No nuclear weapons – no 70-years of global peace (or maybe: no eventual world destruction?).
I can think of exactly three people over the course of human history who I’m fairly confident had a large (the first two, positive) impact on the world: Socrates, Jesus, Marx.
Socrates was sentenced to capital punishment by the Athenians and we only know about him because of Plato.
Jesus died on the cross, with both Jews and Romans mocking him for not being able to get off it.
Marx spent the last 30 years of his life in exile, didn’t even finish writing Das Kapital, and his funeral was attended by seven people.
Truth is, nobody knows the impact of anything they do. As soon as you start thinking about impact, you either start lying to yourself or go insane.
Sometimes people try to talk about estimating probabilities, but I feel like that’s kind of dumb.
We have history. There’s no probabilities there. We simply don’t know what kind of impact anything or anyone really had in the long-term.
But I think it gets worse.
Socrates wasn’t trying to teach all of the Western Civilization how to think: he was just being annoying to everyone, asking questions.
Jesus was trying to become the king of the Jews (Matthew 2:2), but ended up being crucified as a false messiah by them, yet accepted by billions of goys.
None of Marx’s stirring up communist revolutions worked and only because of the Prussian government getting tired of him and exiling him to London was he able to start the work that actually ended up causing communist revolutions and showing to the entire world what building communism actually looks like.
Anyone who decides to do or not to do things based on their impact is bullshitting themselves; and anyone who tells you to do things because they’re high-impact or not do them because they’re low-impact is bullshitting you.
So what should we do with our lives? I wrote recently that I’m probably literally the worst person in the world to be asking this question, but my conclusion– at least for now– is pretty straightforward:
That’s it.
2001-01-01 08:00:00
A few very embarrassing poems I wrote when I was 18, after watching too much battle rap (Russian example; American example) and getting very inspired, trying to impress a couple girls I had crushes on (unsuccessfully)…
I will be an artist, true master of craft.
occupation by art–my whole-hearted part
in this morbid movie, with one sorry actor.
when water turned vapor, all choices dried up.
masturbation sublime, last exultation of mine.
maturation gone by: past taught but a dime.
but who’s in the limelight half kilo off time?
not I.
[context: the girl I was trying to impress liked the writing of Dostoyevsky, Salinger, Hesse, and Hewingway; and films of Bergstrom, Tarkovsky, and Fellini]
Which one do I pick? How can I decide?
‘stoevsky with psych or Salinger’s cries?
The first is too quaint; latter too trite.
Salinger’s trite? No way this is right!
Whatever, who’s next? The judgement is nigh.
Glassbead was nice, no questions on that.
Vocab though – nightmarish (to Hesse’s delight).
‘mingway’s hour of pride: What’s got he for us?
4 wives; 3 wars; shotgun; suicide.
Writing pithy and forceful. Not much can I cite.
The others? Be honest: Don’t know – cannot write.
Okay, writers done. Can filmmakers fight?
No need: Seventh’s Seal is too bright;
the rest are in fright and scrambling for light.
Rip Tarkovsky, Fellini, and also rip rhyme.
Regardless, don’t care, I’m running out of time.
читаю свой рэп быстро
будто это хладнокровное убийство
эминем, оксимирон мне нипочём;
их хип-хап кидаю через плечо
чёткие раймы, вам не ломаный речитатив
эмси молодой кинь мне качовый риф, йо
спасибо центру за это
иду по арбату в кафе на угле
скейт под ногами, попа в руке
кидаю строчки и взгляды
как стальные катаны и нагинаты
испаряют прохожих, как копов наряды
бит всё мощнее; три полоски на мне,
буду шагать, ведь олдскул жив на земле
спасибо центру за это
painter’s from pain, cause art is a torment.
you try; next you sweat; then start crying;
if lucky, then new, something great sees the light
if not, which is always, the next day it might.